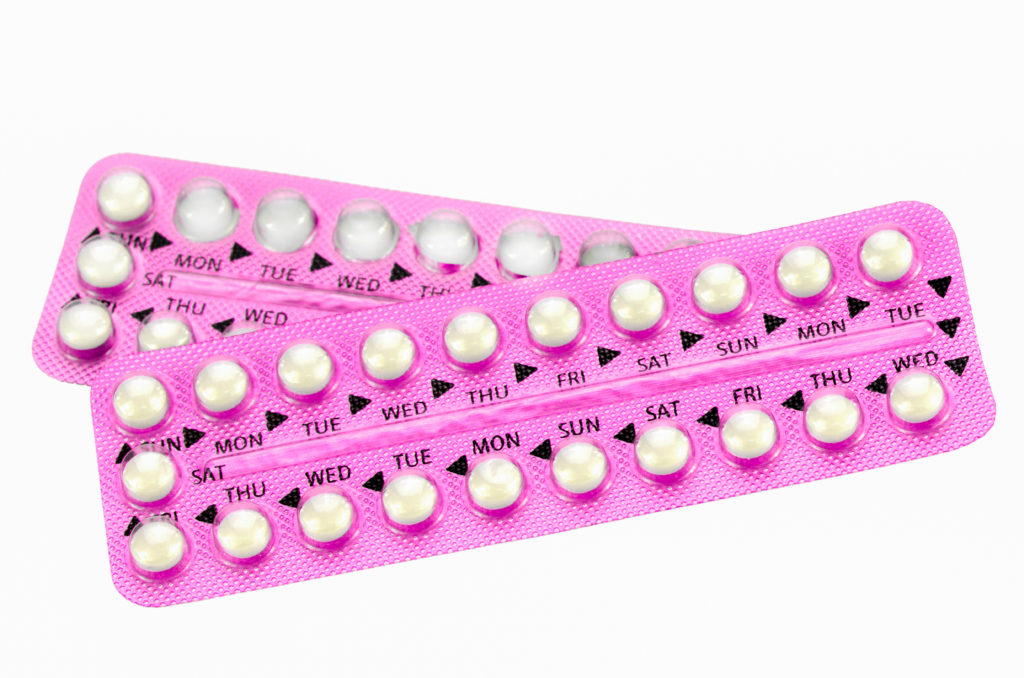
Taking ‘the pill’. A different approach to make this method work best for you
posted by: Jonathan Shaw
Many women worldwide take the combined pill as their main method of contraception. It is not only a reliable method of contraception when taken properly but has added benefits in helping with painful heavy periods and acne. Despite longer acting methods of contraception such as implants and intrauterine methods (“coils”) being more effective than the pill some women do not want to use these methods (which have to be fitted and removed by a healthcare professional) but choose to use the combined pill. These women should be helped to understand how the pill works and how they can take it to make it as effective and convenient for them as possible.
The “pill” was developed back in the 1950s with the intent to mimic the natural female cycle. It was believed that women would want to have a monthly period so it was designed to be taken for 21 days followed by a 7 day break during which there would be a bleed. This regime is still the licensed or usual way to take the pill today but we now understand so much more about how it works and how we can make it work better for the women who use it.
It was first used in the USA in 1960 and it arrived on the scene in the UK in 1961. It is fair to say that it transformed many women’s lives and enabled the sexual revolution that then took place in the 60s. Women had the means to control their fertility (as long as they were married and had their husband’s permission but that is another story…). Over the decades the pill has evolved with lower doses and different combinations of hormones. The low dose pills used today are safe and effective and are the only method of hormonal contraception which results in a regular predictable bleed pattern. This is one of the main advantages of the combined pill and probably why it remains so popular.
The bleed that occurs in the pill free break however is not a proper period. The natural cycle is switched off by the pill so women do not ovulate (release an egg) and the bleed at the end of each packet is nothing more than a hormone withdrawal bleed due to having stopped the pill. This bleed is not necessary for medical reasons and there are definite advantages in avoiding it.
Let’s look at how the pill works. It takes seven days of pill taking to “switch off” the ovaries and stop ovulation occurring. During the 7 day pill free break at the end of each packet the dose of the pill in the body is reducing and the ovaries begin to “wake up” and by the end of the 7 day break some women are very close to ovulating. In fact we know now that some women will release an egg the very next day if they do not restart their next packet on time. So in other words, the pill is at its weakest at the end of the break each month. This is why it is so important to start each packet on time and to never allow the break to become longer than seven days. This does not allow for much leeway though and it seems a little risky for this to potentially happen every month.
So why do we need a break at all? And why does it have to be 7 days? Well, if the pill is taken continuously with no breaks it is very likely that the lining of the womb will thicken a little and start to shed randomly which will result in irregular spotting and bleeding. We call this break-through bleeding. This is exactly what women using the combined pill do not want and do not have to put up with. But women can reduce the number of breaks they have or they can shorten the break to 4 days instead of 7 thereby reducing the potential number of risky times per year. This may therefore make the pill less likely to fail.
The other benefit is obvious- less bleeds. As said these bleeds are not proper periods, they do not serve any medical purpose and contrary to belief they cannot be taken to mean the woman is not pregnant. In fact women who become pregnant on the pill often still have a bleed in the pill free week and this can lull some women into a false sense of security. There are other myths too about the role of “pill periods”- some women worry about where the blood goes and feel the need to “flush” the womb. The truth is the lining of the womb does not thicken up when on the pill to the same extend as in a normal female cycle so therefore there is no blood to lose.
And surely it is worth saving money on tampons and pads? Particularly with VAT applied as it still is sadly (but that’s another story too….)
There is evidence that taking the pill in a continuous or extended way is very acceptable to women in terms of side effects being similar to those with the usual regime and some women find less trouble with headaches, bloating and period pain when taken this way.
The Faculty of Sexual health and Reproductive Healthcare supports the use of extended or continuous regimes. Although these regimes are unlicensed and there is no evidence on the long term health effects of taking the pill in this way, based on how the pill works there is no evidence to suggest it could be harmful. It is recognised that some women like taking their pill in the usual way and if doing this works for them then they should continue. If however they would like to skip bleeds and would like to reduce the chance of ovulation then these regimes can be tried:
- Run together packets. Women often do this to avoid periods on holiday and it is fine to do.For example, take 3 packets of pills (3 x 21 tablets) in a row and then have a 4 day break. Some women can run more than 3 packets together before break through bleeding starts and some prefer to run together just 2 packets.
- Take the pill every day until break through bleeding occurs. If persistent spotting or bleeding occurs for 3 days in a row take this as a sign that it is time for a break and then take a 4 day break. A break must not be taken more than once a month though.
These regimes are flexible and different women will find different regimes work best for them. Both allow women to take a planned break and have a bleed when convenient for them.
The important rules to remember are:
- Never have more than one break a month and never take a break longer than 7 days (this is the licensed pill taking regime). Having less breaks and shorter breaks is fine.
- And, if you miss pills then you should take at least 7 pills correctly before taking your next planned break.
Why not give it a go? Remember this only applies to combined pills, not progesterone only pills.
If you would like any further advice on this please given us a ring on 0300 303 3989.

Get set for summer!
Heading to a festival this summer? Have safer festival fun by signing up for the Eddystone Trust free condoms for […]

Bank Holiday information
All Devon Sexual Health clinics will be closed on Monday 27th May for the Bank Holiday. When our clinics are […]

#StopItNow campaign returns this March
The Stop It Now campaign is aimed at deterring online child sexual abuse. The campaign is a project of the […]

New time for Exeter Young Person clinic.
From 4 March, the Young Person drop-in clinic at Devon Sexual Health will be held every Tuesday from 3.30pm – […]